From Food Pyramids to Real Food: What 50 Years of Changing Nutrition Advice Teaches Us
By Terry Tebbs | Well & Whole
If you grew up in the 1980s or 1990s, you probably remember being told to avoid eggs, switch from butter to margarine, and build your diet on a foundation of bread, pasta, and cereal. The food pyramid—with grains at its wide base and fats at its tiny peak—was gospel.
On January 7, 2026, the U.S. government released new Dietary Guidelines for Americans that would have shocked that earlier generation of nutritionists. The message is now remarkably simple: eat real food.
The 2025-2030 guidelines represent what Health Secretary Robert F. Kennedy Jr. called “the most significant reset of federal nutrition policy in decades.” But for many Americans, the bigger question isn’t what changed—it’s why our nutritional guidance keeps changing, and how we’re supposed to know what to believe.
What the New Guidelines Actually Say
The new Dietary Guidelines for Americans can be summarized in a few key principles:
Prioritize whole, nutrient-dense foods. The guidelines emphasize protein, dairy, vegetables, fruits, healthy fats, and whole grains—in roughly that order of priority.
Avoid highly processed foods. For the first time, federal dietary guidance explicitly calls out ultra-processed foods as a category to limit, including those “laden with refined carbohydrates, added sugars, excess sodium, unhealthy fats, and chemical additives.”
Full-fat dairy is back. The guidelines recommend three servings of dairy daily and no longer push low-fat versions as the default choice.
Eggs are encouraged. There’s no longer any mention of limiting dietary cholesterol, and eggs are positioned as a nutrient-rich whole food appropriate across the lifespan.
Butter and beef tallow are listed as cooking options. Alongside olive oil, these traditional fats—long demonized—are now mentioned as “healthy fat” choices.
The saturated fat limit remains. Despite the emphasis on whole-food fats, the guidelines retain the recommendation to limit saturated fat to no more than 10% of daily calories.
That last point has created some confusion. How can butter be recommended while saturated fat is limited? Harvard nutrition professor Frank Hu noted that “the mixed messages surrounding saturated-fat-rich foods such as red meat, butter, and beef tallow may lead to confusion.”
How We Got Here: A Brief History of American Dietary Advice
To understand where we are, we need to understand where we’ve been.
The 1970s: Fat Becomes the Enemy
In 1977, a Senate committee led by Senator George McGovern released “Dietary Goals for the United States,” recommending Americans consume less fat, saturated fat, and cholesterol—and more carbohydrates. This marked a dramatic shift. As the focus turned to heart disease prevention, dietary fat became increasingly suspect.
The thinking at the time seemed logical: if fatty deposits clog arteries, eating less fat should help. But as Dariush Mozaffarian, dean of the Friedman School of Nutrition Science and Policy at Tufts University, later explained, “We know now that carbohydrates worsen glucose and insulin—they have negative effects on blood cholesterol levels.”
1980: The First Dietary Guidelines
The first official Dietary Guidelines for Americans emphasized a diet low in fat, saturated fat, and cholesterol. Americans were advised to limit egg consumption to two or three per week. Butter was out; margarine was in.
1992: The Food Pyramid Era
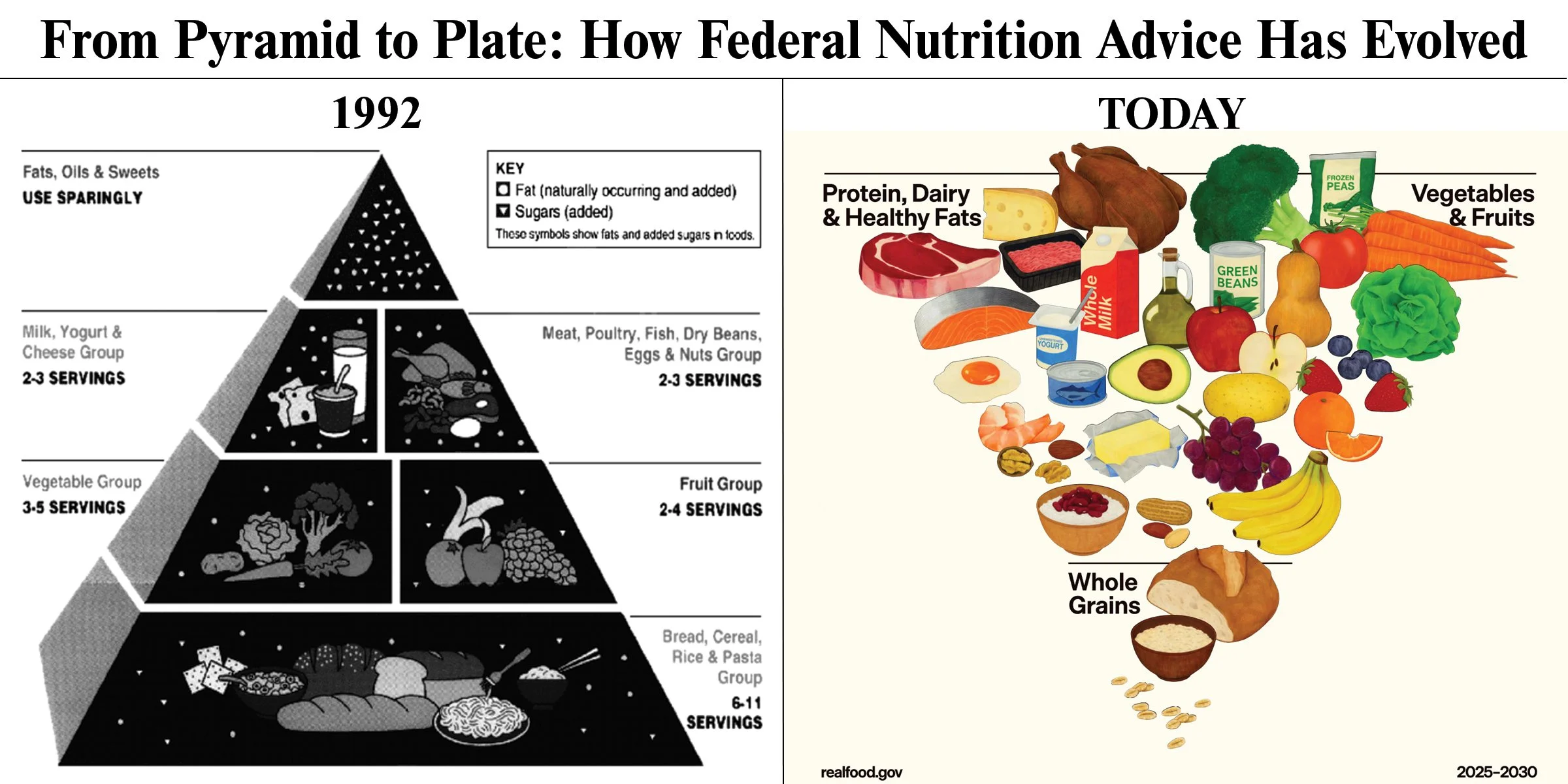
The iconic Food Guide Pyramid placed grains at its base, recommending 6-11 servings daily of bread, pasta, rice, and cereal. Fats and oils sat at the tiny apex with the instruction to “use sparingly.”
The result? Americans dutifully reduced their fat intake and increased carbohydrates. Food manufacturers responded with a flood of “low-fat” and “fat-free” products—often loaded with added sugar to compensate for taste. The low-fat cookie became a cultural phenomenon.
Meanwhile, rates of obesity and diabetes climbed steadily.
2015: The Cholesterol Reversal
The 2015-2020 Dietary Guidelines quietly made a significant change: they removed the longstanding limit of 300 mg of dietary cholesterol per day—a limit that had been in place since 1968. The scientific advisory committee acknowledged that dietary cholesterol was “no longer a nutrient of concern.”
This was a remarkable about-face. For nearly 50 years, Americans had been told to limit eggs. Suddenly, eggs were fine.
The Egg Story: A Case Study in Changing Science
The egg’s journey from villain to hero illustrates how nutritional understanding evolves. (Photo from Adobe Stock by alter_photo)
For decades, the reasoning seemed straightforward: eggs contain cholesterol, high blood cholesterol is associated with heart disease, therefore eating eggs must be bad for your heart. But this logic had a flaw. It assumed that dietary cholesterol directly translates to blood cholesterol—and newer research showed that connection was much weaker than believed.
A 2025 randomized controlled trial published in the American Journal of Clinical Nutrition examined this directly. Researchers found that “saturated fat intake was positively correlated with LDL cholesterol, whereas dietary cholesterol was not.” In fact, participants eating two eggs daily as part of a low-saturated-fat diet actually had lower LDL cholesterol than those eating a high-saturated-fat diet with just one egg per week.
The Framingham Offspring Study, which followed nearly 2,000 adults, found that “consuming five or more eggs per week was not adversely associated with lipid outcomes.” Among men, higher egg consumption was actually associated with lower total cholesterol and LDL cholesterol levels.
Yet despite these findings—and despite the removal of cholesterol limits from official guidelines a decade ago—research shows that outdated advice still shapes behavior. A 2025 study tracking 48 years of eating patterns found that egg consumption dropped from 3.6 eggs per week in the early 1970s to just 1.8 eggs per week by the late 1980s in response to dietary guidance. The study noted that “public health messaging lags behind science.”
Why Nutrition Science Changes
It’s tempting to conclude that nutritionists simply don’t know what they’re talking about. But the reality is more nuanced.
Early studies had limitations. Much of the original research linking dietary fat to heart disease relied on observational studies, which can show correlation but not causation. It took decades to conduct the long-term, controlled trials needed to challenge established assumptions.
The body is complex. Researchers once thought in simple, linear terms: eat fat, get fat; eat cholesterol, get high cholesterol. We now understand that metabolism involves countless interacting systems. How your body processes food depends on what else you eat, your genetics, your gut microbiome, your activity level, and numerous other factors.
Context matters. An egg cooked in butter and served alongside bacon affects the body differently than an egg scrambled with vegetables and olive oil. Early nutrition research often failed to account for these contextual factors.
Science is self-correcting. The process can be frustratingly slow, but the willingness to revise conclusions based on new evidence is a feature of good science, not a bug. As the Harvard T.H. Chan School of Public Health noted, guidelines “reflect the nutrition science of their time.”
What Experts Agree On
Despite ongoing debates about saturated fat and specific foods, there’s remarkable consensus on several points:
Whole foods beat processed foods. Virtually every nutrition expert agrees that minimally processed foods—vegetables, fruits, nuts, legumes, whole grains, quality proteins—should form the foundation of a healthy diet.
Added sugar is problematic. The new guidelines recommend limiting added sugars to less than 6% of daily calories (down from 10% in previous editions). This is one area where the evidence is strong and consistent.
Refined carbohydrates cause problems. The low-fat era’s emphasis on bread and pasta overlooked the metabolic impact of refined grains. There’s now broad agreement that whole grains are preferable and that refined carbohydrates should be limited.
Overall dietary patterns matter more than individual foods. Obsessing over whether eggs or butter are “good” or “bad” misses the point. What matters is the totality of what you eat, how it’s prepared, and how it fits into your lifestyle.
Finding Facts Through the Noise
With nutrition advice seemingly changing constantly and social media full of conflicting claims, how can ordinary people know what to believe?
Look for government and academic sources. The National Institutes of Health (NIH), Centers for Disease Control (CDC), and major academic medical centers base their recommendations on peer-reviewed research. Websites ending in .gov are generally reliable starting points.
Check for citations. Trustworthy health information websites share their sources. Be wary of claims without references to published research.
Watch for red flags. The NIH warns consumers to “be cautious about websites claiming any single remedy will cure many different illnesses” and to be wary of “simple or unproven treatments.” If something sounds too good to be true, it probably is.
Consider the source’s expertise. There’s a difference between content written by a credentialed professional with published research and claims from social media influencers—no matter how many followers they have.
Talk to healthcare providers. Before making significant dietary changes based on anything you read—including official guidelines—consult with your doctor or a registered dietitian who knows your individual health situation.
Looking Ahead: What Might the Next 50 Years Bring?
If the past half-century teaches us anything, it’s humility about predicting the future of nutrition science. But current research points to several directions that may reshape dietary guidance in coming decades.
Personalized nutrition. Advances in genetic testing and microbiome analysis suggest that the future of dietary advice may be highly individualized. What’s optimal for one person’s metabolism may not be optimal for another’s.
Focus on metabolic health. Rather than simply counting calories or fat grams, researchers are increasingly interested in metabolic markers—insulin sensitivity, inflammation, gut health—that may better predict health outcomes.
The ultra-processed food question. While the 2025-2030 guidelines mention processed foods, there’s ongoing scientific debate about how to define and regulate this category. Expect this to be a major focus in coming years.
Sustainability considerations. Future guidelines may need to balance individual nutrition with environmental impact, potentially affecting recommendations around meat consumption and food sourcing.
Artificial intelligence and big data. The ability to analyze massive datasets may reveal patterns in nutrition and health that have eluded traditional research methods.
The Bottom Line
The new Dietary Guidelines for Americans represent a meaningful shift toward whole foods and away from the processed, low-fat products that dominated the previous era. But they also remind us that nutrition science is evolving—and that today’s certainties may be tomorrow’s revisions.
Perhaps the most enduring advice is also the simplest: eat real food, mostly plants, not too much. That guidance, offered by journalist Michael Pollan years ago, captures what remains consistent across changing guidelines.
The details will continue to shift as research advances. But the principle of favoring whole, minimally processed foods over engineered products has held up remarkably well—and seems likely to endure, whatever the next 50 years may bring.
For more wellness content, visit mountainandmain-ut.com. Do you have questions about navigating nutrition advice? Email us at mountainandmain.ut@gmail.com.
Sources
Government Sources: - U.S. Department of Agriculture and U.S. Department of Health and Human Services. Dietary Guidelines for Americans, 2025-2030. Released January 7, 2026. Available at DietaryGuidelines.gov and realfood.gov. - Centers for Disease Control and Prevention. “Benefits of Physical Activity.” Updated December 4, 2025. - National Institute on Aging. “How To Find Reliable Health Information Online.” - Scientific Report of the 2025 Dietary Guidelines Advisory Committee, December 2024.
Peer-Reviewed Research: - Carter S, Hill AM, et al. “Impact of dietary cholesterol from eggs and saturated fat on LDL cholesterol levels: a randomized cross-over study.” American Journal of Clinical Nutrition, 2025. - Framingham Offspring Study findings on eggs and lipid levels. Current Developments in Nutrition, 2024. - Kritz-Silverstein D, Bettencourt R. “Egg Consumption: Trends Over 48 Years, Patterns Across the Lifespan, and Predictors of Intake.” Nutrients, 2025.
Expert Commentary: - Harvard T.H. Chan School of Public Health. “Understanding the new Dietary Guidelines for Americans.” January 2026. - American Heart Association. “Here’s the latest on dietary cholesterol and how it fits in with a healthy diet.” - Mozaffarian D, Friedman School of Nutrition Science and Policy, Tufts University. - Van Horn L, Northwestern University Feinberg School of Medicine.
Historical Context: - Davis C, Saltos E. “Dietary Recommendations and How They Have Changed Over Time.” America’s Eating Habits: Changes and Consequences, USDA Economic Research Service. - “The History and Future of Dietary Guidance in America.” PubMed Central. - NPR. “Wheels, Pyramids And Plates: USDA’s Struggles To Illustrate Good Diet.”